Glaucoma Treatment
Glaucoma is a disease of the optic nerve. It is most often a slowly progressing loss of sight that is not detected by the patient until it has reached advanced stages. The loss of vision begins in the peripheral visual field and only affects the central clear vision in its advanced stages. Because there are no signs or symptoms for the patient to detect, glaucoma is almost always found by an eye doctor during a thorough eye exam.
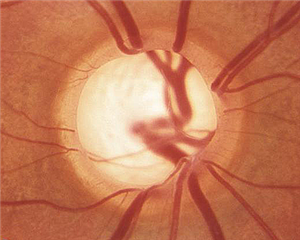
Glaucoma Testing / Detection
Glaucoma can be found by checking the eye’s pressure. Normal eye pressures range from 12 to 21. Glaucoma patients often have pressures higher than the normal range. However, it is possible to have glaucoma and a pressure that is in the normal range. It is also possible to have an elevated eye pressure and not have damage to the optic nerve. Thus, pressure alone is not sufficient to determine whether or not someone has glaucoma; it is only part of the equation. Quick screening exams that only check vision or eye pressure and lack a doctor evaluating the optic nerve can miss glaucoma. Additionally, it is very important to know the thickness of the patient’s cornea. We use a device called an ultrasound pachymeter to measure corneal thickness. Thicker corneas will give erroneously high pressure readings and thin corneas will be erroneously low. Thus corneal thickness is an important part of glaucoma diagnosis and treatment.
The examining eye doctor can look into the anterior part of the eye with a special mirror lens. This test is called gonioscopy. It should be performed initially on glaucoma suspects to see if there is a physical blockage of the eye’s drainage system called the trabecular meshwork. If the drainage angle is narrow, eye dilation can be dangerous until a laser can be used to treat this condition. The eye pressure can be reduced in many narrow angle cases by laser treatment.
Visual field testing checks how sensitive our side vision is and compares it to a database of normal patients. This is the gold standard test and it should be done yearly on all glaucoma patients. Anyone suspicious for glaucoma should have a visual field test as well. If there is significant damage to the optic nerve it shows up as a loss of sensitivity in the side vision (which by the way is not noticed by the patient). It has been shown that a large portion of the nerve fibers in the optic nerve must be lost before the visual field test can detect glaucoma. Some studies have suggested as many as 30 to 50% of the nearly 1.2 million nerve fibers are lost before standard visual field tests can detect the loss. This has led eye doctors to search for more sensitive testing to try and find glaucoma earlier. Early detection and treatment would thus spare more of the optic nerve.
In addition to testing the visual field, there are optic nerve analyzers that use scanning lasers to take precise measurements of the optic nerve and surrounding nerve fibers. These remarkable devices give vary accurate objective information regarding the shape and thickness of the optic nerve and compare it to the normal population data helping to diagnose glaucoma and monitor for further optic nerve damage over time. The optic nerve and retinal nerve fiber layer analysis can be repeated later (1 year. Optic nerve analysis not only helps in making the diagnosis of glaucoma, but it also helps determine if the current treatment is adequately preventing further damage for those already receiving treatment for glaucoma.
Glaucoma Treatment
Medical Treatment
Glaucoma is treated by lowering the eye pressure. This is most often done with eye drop medications. There are several classes of drops, some decrease eye fluid production, others increase the outflow of flow; both resulting in lower eye pressure. If one type of glaucoma drop does not lower the pressure enough, additional glaucoma medication(s) may be required.
Laser Treatment
Glaucoma eye drops can be expensive and many have unwanted side effects. Laser treatment is often used as an alternative to eye drops, or to lower eye pressure more when the patient’s current eye medications are not lowering the pressure enough.
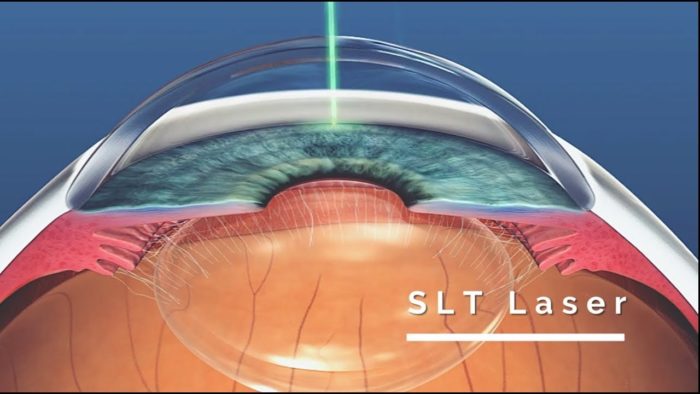
Selective Laser Trabeculoplasty, or SLT, is a laser treatment that can be applied in a few minutes to lower eye pressure and treat glaucoma. The eye pressure is lowered in about 70% of the patients treated. Many glaucoma patients can reduce their dependency on drops by having this laser applied.
The benefits of SLT include no systemic side effects or compliance issues encountered with eye drops. The SLT treatment is “selective”, targeting only cells with melanin, there is no anatomic thermal damage to the surrounding trabecular meshwork as seen with prior laser techniques such as Argon Laser Trabeculoplasty (ALT). Thus, SLT can be repeated in the future if needed.
Patients enjoy the long-term savings by reducing their dependency on expensive eye drops. Most patients find SLT laser to be a quick and painless procedure for glaucoma. SLT is reimbursed by Medicare and most insurances.
Surgical Treatment
Recently there have been technologic advances for better control of the intraocular pressure. Minimally invasive glaucoma surgical procedures, so-called MIGS procedures, involve alterations of the drainage area that are performed inside the eye. There are several options, two of our favorites are the iStent Inject and the XEN gel stent.
The iStent is designed to improve the outflow of fluid to better lower the intraocular pressure and possibly reduce the need for medications. The iStent is the smallest medical device approved by the FDA to date. Typically, two small iStent implants are placed in your eye into the drainage area, called the trabecular meshwork, at the time of cataract surgery.


The XEN Gel Stent is another new MIGS device that can be surgically implant for more advanced glaucoma that is not responding well to glaucoma eye drops.
There are more invasive procedures (e.g., trabeculectomy or Express shunt) that can be done for advanced glaucoma that is not responding to medical, laser or MIGS treatments.
And finally, there is a laser that can be applied at the time of cataract surgery to decease the production of fluid in the eye and lower the eye pressure called Endocyclophotocoagulation, ECP. Dr. Strickler performs ECP on glaucoma patients that elect it at the time of cataract surgery.
Payment Options
You can use your Health Care Savings Account (HSA) or Flex Spending Account to help cover the additional cost of Glaucoma Surgery; this saves you money by using pretax dollars. Financing can often be arranged for those who qualify by Care Credit. Contact us today to learn more about payment options.
